At the time of writing, there have been almost a quarter of a million confirmed cases of COVID-19 worldwide. The number of deaths is approaching 10,000. Across the world, countries are scrambling to increase their testing capacity for the virus.
How are these tests carried out and how do they work?
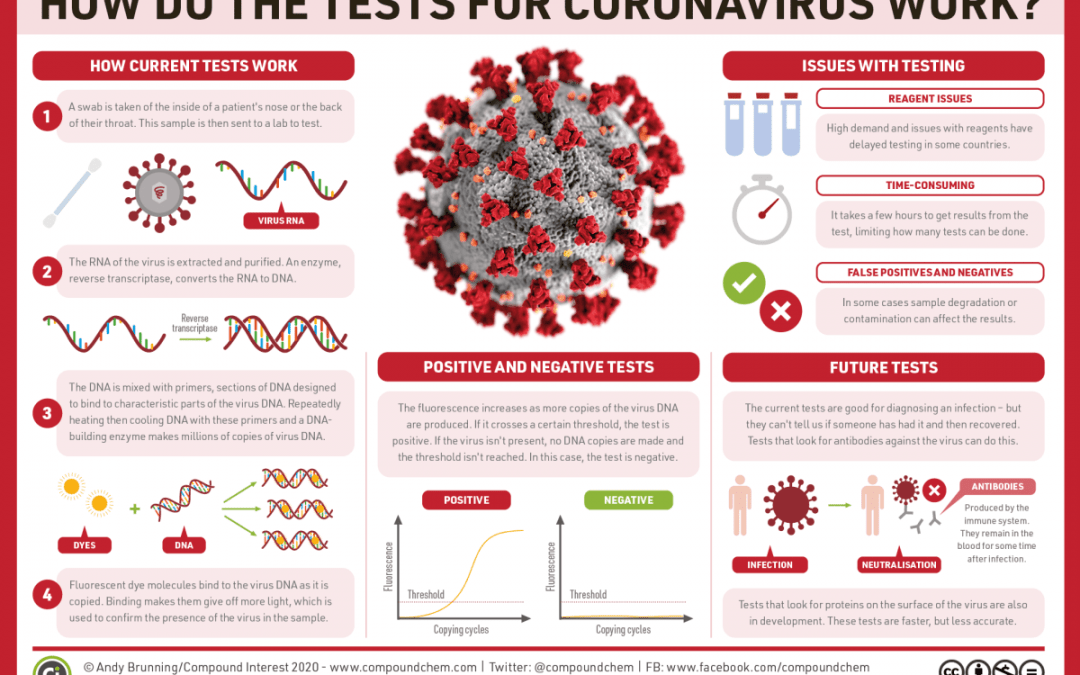
The tests currently being used to identify coronavirus infection are known as PCR tests. PCR stands for ‘polymerase chain reaction’, and it’s by no means a new testing method — PCR tests have been used since the 1980s and have a range of applications including the diagnosis of infectious diseases. The tests allow copying of a small amount of DNA millions of times over so that there is enough for detection and confirmation of infection.
Testing for the virus needs a sample. First, a swab is taken, usually from a patient’s nose or the back of their throat. The swab is then placed in a secure container and sent to a laboratory for further analysis. Analysis needs to take place within a few days of the sample being taken.
DNA makes up our genetic material and that of some types of viruses. But the virus which causes COVID-19, SARS-CoV-19, does not contain double-stranded DNA, but single-stranded RNA. As the PCR tests can only make copies of DNA, we need to convert the RNA into DNA first.
The virus RNA is extracted from the swab sample. It then needs to be purified from the human cells and enzymes which may otherwise interfere with the PCR test. Often, labs use kits made by chemical suppliers specifically for this purpose to do this.
The purified RNA is mixed with an enzyme called reverse transcriptase. This enzyme converts the one-stranded RNA to double-stranded DNA so that it can be used in the PCR test.
The virus DNA is then added to a test tube to which the following are also added:
- Primers: these are short sections of DNA designed to bind to characteristic parts of the virus DNA. Because of this they won’t bind to DNA which isn’t from the virus.
- Nucleotides: these are the building blocks that make up DNA.
- A DNA-building enzyme: this makes copies of the DNA.
A PCR machine heats the mixture. This causes the double-stranded DNA to unravel, and the primer can then bind to the DNA as it cools. Once the primers have bound to the DNA, they provide a starting point for the DNA-building enzyme to help copy it. This process continues through repeated heating and cooling until millions of copies of the DNA have been created.
This explains how PCR amplifies the virus genetic code, but not how it’s detected. This is where fluorescent dyes, added to the test tube while the DNA is being copied, come in. They bind to the copied DNA, which boosts their fluorescence, making them give off more light. It’s this light which allows us to confirm the presence of the virus.
The fluorescence increases as more copies of the virus DNA are produced. If the fluorescence crosses a certain threshold, set above expected background levels, the test is positive. If the virus wasn’t present in the sample, the PCR test won’t have made copies, so the fluorescence threshold isn’t reached — the test is negative.
Though they may sound complex, PCR tests are a pretty reliable way of testing for infectious diseases, which is why they’re used widely to test for COVID-19. However, some countries have run into issues when trying to scale up their testing capabilities.
One reason for this is simply the fact that the test takes time. It can take a few hours to get results; couple this with lab testing capacities and it places a limit on how many tests a single lab can carry out in a day. A small research lab might be able to run around 80 tests a day; much larger labs with multiple machines may be able to run between 1000-2000.
Another limitation is the availability of reagents needed to run the tests. We mentioned previously that some companies sell RNA extraction kits for this step of the process. Global demand for these tests in the wake of the pandemic has led to a shortage, limiting the number of tests carried out.
In some cases, the tests haven’t functioned as intended. The tests originally provided for diagnosis in the USA contained different sets of primers for different purposes. This included one which targeted a genetic sequence found in all coronaviruses as a form of control test. This part of the test didn’t function correctly; while it didn’t stop them from being usable, it caused confusion as to whether results were positive or not, slowing diagnosis.
Contamination or degradation can also cause issues. These can lead to false positives (when someone doesn’t have the virus but the test says they do) or false negatives (when someone does have the virus but the test says they don’t).
A final big limitation of this type of testing is that it can only tell you if someone has the virus at the time of testing. It can’t tell us whether they’ve had the virus but have subsequently recovered before testing. This is pretty useful to know, as if someone’s had the virus and recovered, they’ll be immune to catching it again (at least for a while).
A type of test that can tell us whether someone has previously had the virus is an antibody-based test. Your body produces antibodies to fight off infections. These antibodies remain in your blood for some time after infection, and tests can detect them. Currently, some companies are working on antibody tests for the SARS-CoV-2 virus, and it’s expected that they’ll be rolled out quickly once they’re available.
There are other tests which could prove useful too. Another type looks for specific proteins on the surface of viruses. They’re faster than the PCR testing, but also less sensitive, so there’s more chance of an inaccurate result.
The World Health Organisation has stressed the importance of testing as part of the worldwide response to the COVID-19 pandemic. There’s significant variability in the number of tests carried out in different countries. China and South Korea have both run around 300,000 tests, whereas the United Kingdom and the United States have only run 50,000 and 40,000 respectively. Less testing means it’s harder to track the spread of the infection and isolate and track contacts of the infected.
Until testing capacity increases and more types of test become available, countries are advising their citizens to self-isolate if they think they may have symptoms of the virus. Some may only know for sure if they’ve had the virus once antibody tests are available, but following this advice and that on social distancing is the best way to prevent its spread.
Remember, while you may not be in one of the groups most at risk of serious complications or death from the virus, your actions could prevent you from passing it on to someone who is. And really, staying in your house for a few weeks seems like a small price to pay to save a life.